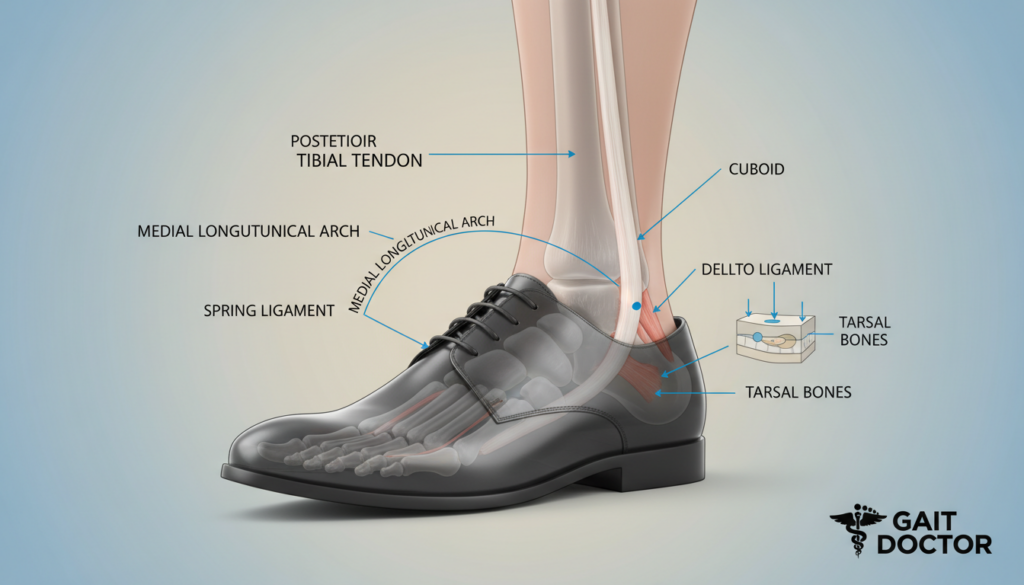
The tibial tendon is key in keeping the foot’s arch up. If it fails, it can cause posterior tibial tendon dysfunction. This makes the arch fall down.
Gait analysis spots problems in how the foot moves. The Cleveland Clinic says symptoms are pain, swelling, and weakness in the foot or ankle.
Key Takeaways
- Tendon failure can lead to a collapsed arch.
- Gait analysis helps identify potential issues.
- Symptoms include pain and swelling in the foot or ankle.
- Effective management prevents further complications.
- Foot mechanics play a crucial role in this condition.
Table of Contents
ToggleUnderstanding Posterior Tibial Tendon Dysfunction
The posterior tibial tendon is key for foot movement. It supports the arch and helps with walking. This tendon links the calf muscle to the foot’s inside arch.
The Role of the Posterior Tibial Tendon in Foot Mechanics
The tendon is vital for walking right. It keeps the arch supported and the foot aligned. Damage to this tendon can cause many problems.
Some important jobs of the tendon are:
- Supporting the arch of the foot
- Helping with normal walking
- Keeping the foot in the right shape
When the tendon works well, it spreads out foot pressure. This lowers injury risks and flatfoot chances. But, damage or swelling can cause tendon dysfunction.
Posterior tibial tendon dysfunction changes how the foot works. This can cause pain and discomfort. Knowing about the tendon’s role helps in treating this condition.
Experts say, “The posterior tibial tendon is very important for the foot’s arch. When it doesn’t work right, it can cause many symptoms, from mild pain to serious deformity.”
Causes and Risk Factors of Posterior Tibial Tendon Dysfunction
It’s important to know what causes posterior tibial tendon dysfunction. This helps in managing and preventing it. Many things can lead to this condition, like overuse, foot problems, and health issues.
Contributing Factors to Posterior Tibial Tendon Dysfunction
Several things can make you more likely to get posterior tibial tendon dysfunction. Overuse injuries are a big risk, mainly for athletes or those who do lots of repetitive activities. Foot abnormalities, like flat feet or high arches, also increase the risk by changing how the foot works.
Other things that can contribute include:
- Rheumatoid arthritis and other inflammatory conditions
- Diabetes and associated neuropathy
- Obesity, which increases stress on the tendon
- Previous injuries or surgeries affecting the foot or ankle
| Risk Factor | Description | Impact |
|---|---|---|
| Overuse Injuries | Repetitive stress on the tendon | Increases the risk of tendon dysfunction |
| Foot Abnormalities | Flat feet or high arches | Alters foot biomechanics, stressing the tendon |
| Rheumatoid Arthritis | Inflammatory condition | Can cause tendon inflammation and degeneration |
Knowing these risk factors is key for early treatment. Healthcare providers can then make better plans to help with posterior tibial tendon dysfunction.
Recognizing the Signs and Symptoms
It’s important to spot the early signs of posterior tibial tendon dysfunction. This condition shows up in different ways. It can affect how your foot works and how you move around.
Early Warning Signs of Posterior Tibial Tendon Dysfunction
Pain, swelling, and changes in how your foot looks or works are early signs. These symptoms can get worse over time. This can make it hard to walk or stand.
Changes in Foot Appearance and Function
One big change is a flat foot or a collapsed arch. This makes it hard to walk or stand for a long time. Swelling along the inner ankle or foot is another sign you shouldn’t ignore.
The table below lists common signs and symptoms of posterior tibial tendon dysfunction:
| Signs and Symptoms | Description |
|---|---|
| Pain along the posterior tibial tendon | Pain is typically felt along the inner ankle and foot |
| Swelling | Swelling occurs along the inner ankle or foot |
| Changes in foot appearance | Development of a flat foot or collapsed arch |
| Difficulty walking or standing | Increased difficulty in performing daily activities due to foot pain or deformity |
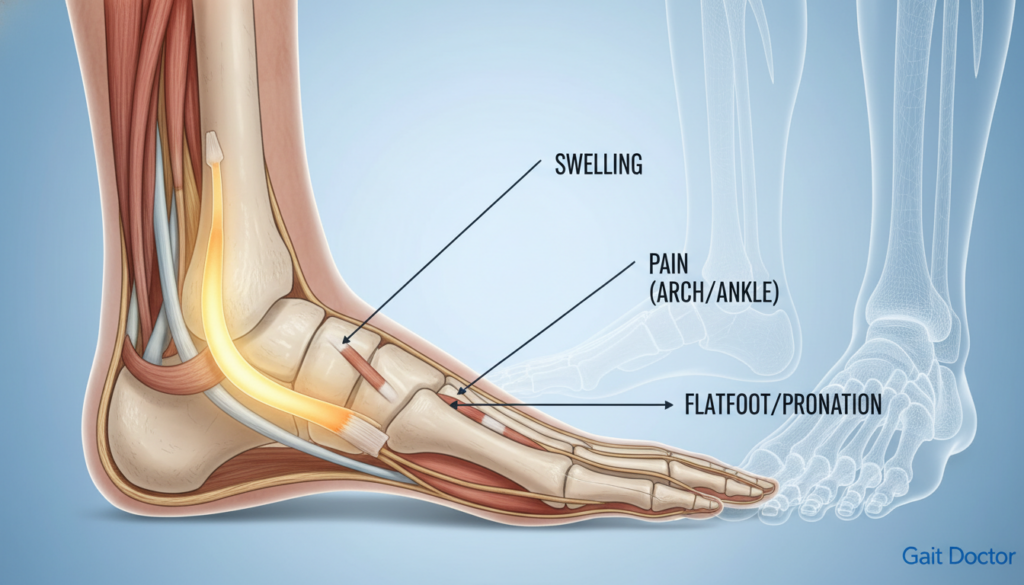
If you notice these symptoms, see a doctor right away. Getting help early can make a big difference. It can help prevent things from getting worse.
Stages of Posterior Tibial Tendon Dysfunction
Posterior Tibial Tendon Dysfunction goes through different stages. Each stage shows how bad the problem is. It helps doctors decide the best treatment.
The first stage is when the tendon starts to hurt. It might feel tight or sore. This is the beginning of the problem.
In the second stage, the tendon gets inflamed. It swells up and hurts more. This makes it hard to move the foot right.
The third stage is when the tendon starts to tear. It might feel weak or like it’s breaking. This is a serious problem that needs quick treatment.
Knowing the stages helps doctors treat the problem better. They can choose the right treatment for each stage. This helps the tendon heal and keeps the foot working right.
Understanding the Stages of Posterior Tibial Tendon Dysfunction
Here’s a table that shows the stages of Posterior Tibial Tendon Dysfunction:
| Stage | Characteristics |
|---|---|
| Stage 1 | Tendon pain and tightness |
| Stage 2 | Tendon inflammation and swelling |
| Stage 3 | Tendon tears and weakness |
Knowing the stages helps doctors treat the problem better. They can choose the right treatment for each stage. This helps the tendon heal and keeps the foot working right.
Diagnosis and Assessment Approaches
Getting a correct diagnosis for posterior tibial tendon dysfunction is key. It needs both clinical checks and imaging. Knowing the exact problem helps doctors choose the right treatment.
Clinical Examination Techniques
Doctors start by checking the foot and ankle. They look for any odd shapes or tenderness. They also check how well the foot moves and the strength of the muscles.
- They look at the foot and ankle for any odd shapes or problems.
- They feel the tendon to see if it hurts.
- They check how well the foot moves.
- They test the strength of the muscles that support the arch.
These checks help doctors understand the tendon’s condition and how bad it is.
Imaging and Advanced Diagnostics
Imaging is also very important. It helps doctors see the extent of the damage. They use:
- X-rays to look at the bones in the foot.
- Ultrasound to see the tendon’s structure and any damage.
- MRI to get detailed pictures of the tendon and nearby tissues.
These advanced images are crucial for diagnosing and treating posterior tibial tendon dysfunction.
Experts say, “Imaging is very important for diagnosing and treating posterior tibial tendon dysfunction. It gives doctors detailed information to make treatment plans.”
The Role of Gait Analysis in Assessing Foot Mechanics
Gait analysis is key in finding foot problems linked to posterior tibial tendon dysfunction. It lets doctors see how a patient walks. They can spot any odd walking patterns.
Knowing how we walk is vital for fixing posterior tibial tendon dysfunction.
How Gait Analysis Can Help Identify Abnormalities in Foot Mechanics
Gait analysis studies how we walk. It uses watching, measuring, and checking our body’s movement. Doctors can find foot problems that cause posterior tibial tendon dysfunction by looking at how we walk.
It can spot overpronation, supination, and other foot movement issues. Spotting these problems early helps treat posterior tibial tendon dysfunction better. Doctors say, “Gait analysis is key for finding the right treatment.”
“Gait analysis is essential for understanding the complex interactions between the foot and the rest of the lower limb during walking.”
Conservative Management Options
Conservative management is key in treating posterior tibial tendon dysfunction. It includes rest, changing how you move, and using supports. Physical therapy also helps strengthen the tendon and improve foot function.
Rest, Activity Modification, and Supportive Devices
Rest and changing how you move are important. They help reduce pain and swelling. Using supports like orthotics or braces also helps a lot.
- Orthotics: Custom orthotics help spread out pressure and support the arch.
- Bracing: Bracing adds extra support to the foot and ankle.
- Shoe Modifications: Changing your shoes to be more supportive can also help.
Physical Therapy and Rehabilitation Strategies
Physical therapy is also very important. A physical therapist can make a plan to strengthen the muscles around the tendon. This improves flexibility and foot mechanics.
Key elements of a physical therapy program may include:
- Strengthening exercises to make the tendon and muscles stronger.
- Flexibility exercises to improve range of motion and reduce stiffness.
- Functional training to better your gait and foot function.
By using these strategies, patients can see big improvements. They might not need more serious treatments.
Custom Orthotics as a Supportive Measure
Custom orthotics are key in managing posterior tibial tendon dysfunction. They offer arch support and improve foot mechanics. This helps a lot with symptoms of PTTD.
How Custom Orthotics Can Support Foot Function
Custom orthotics are made to support the arch and other foot parts. They help spread out pressure and ease the tendon’s strain. This is very helpful in the early stages of PTTD.
Key benefits of custom orthotics for PTTD include:
- Personalized support tailored to the individual’s foot shape
- Redistribution of pressure to alleviate strain on the posterior tibial tendon
- Enhanced foot mechanics to improve overall function and mobility
Adding custom orthotics to a treatment plan can greatly help PTTD patients. It’s important to talk to a healthcare expert. They can find the best orthotics for you based on your needs and how bad your condition is.
Surgical Interventions for Advanced Cases
In advanced cases of Posterior Tibial Tendon Dysfunction, surgery might be needed. This is to fix the deformity and bring back function. Such surgeries can greatly improve life quality for those with this condition.
Surgical Options for Correcting Deformity and Restoring Function
Surgery choices depend on how bad the deformity is and the person’s health. They might fix the heel’s position, stretch the calf muscle, or fuse joints for stability. Each surgery is made just for the patient, aiming for the best results.
Conclusion: Managing Posterior Tibial Tendon Dysfunction
Managing posterior tibial tendon dysfunction well needs a full plan. This plan should include learning, trying conservative methods, and sometimes surgery. Knowing about the condition and how to treat it helps people manage their symptoms better.
Being proactive in prevention and management can help a lot. People can lessen the chance of things getting worse. They can also feel better by using custom orthotics, going to physical therapy, and changing how they move.
Every person needs a treatment plan made just for them. This is key to getting the best results in managing posterior tibial tendon dysfunction.