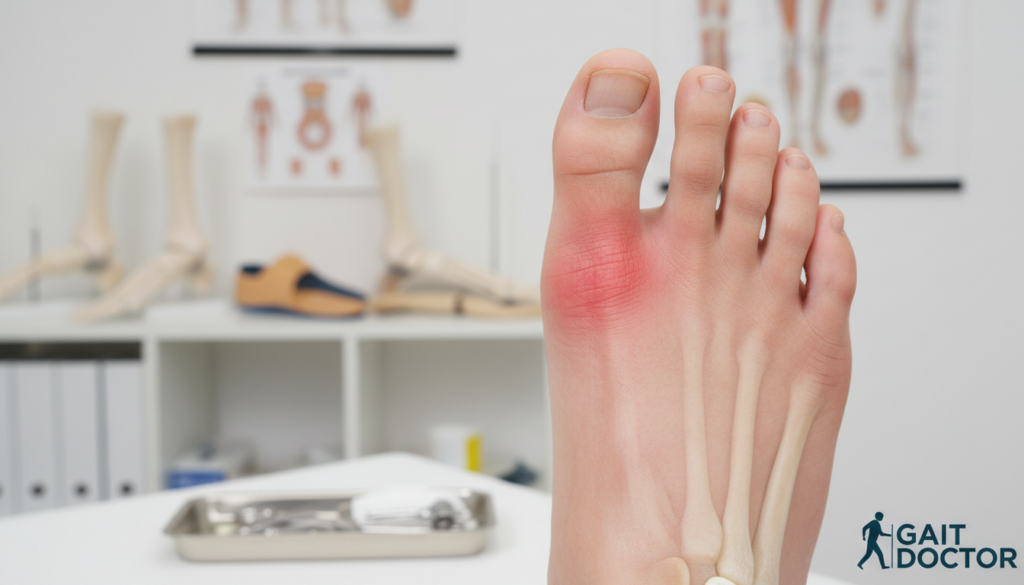
Morton’s Neuroma is a condition that affects the nerves in the foot. It causes pain and discomfort. The tissue around the nerves gets thick, leading to irritation and pain.
Common symptoms include sharp, burning pain in the ball of the foot. You might also feel numbness or tingling. Walking or standing can be uncomfortable.
It’s important to recognize these symptoms early for relief. If not treated, Morton’s Neuroma can cause long-lasting foot pain. It can also make daily activities hard.
Key Takeaways
- Understanding Morton’s Neuroma is key to managing its symptoms.
- Common symptoms include sharp pain and numbness in the foot.
- Timely recognition of symptoms is crucial for effective relief.
- Untreated Morton’s Neuroma can lead to persistent foot pain.
- Seeking professional help is essential for proper diagnosis and treatment.
Table of Contents
ToggleUnderstanding Morton’s Neuroma
To understand Morton’s Neuroma, we need to know its basics. It’s not a tumor but a condition. It makes the tissue around a nerve in the foot thick. This leads to pain and discomfort.
What Is Morton’s Neuroma?
Morton’s Neuroma is when the tissue around the nerves between the toes gets thick. This usually happens between the third and fourth toes. This thickening irritates the nerve, causing pain.
How Common Is This Condition?
Morton’s Neuroma is quite common. It affects runners and people who wear high heels or tight shoes. The table below shows how common it is in different groups.
| Population | Prevalence |
|---|---|
| Runners | High |
| Individuals wearing high heels | Moderate to High |
| General Population | Low to Moderate |
The Anatomy of Morton’s Neuroma
Morton’s Neuroma happens because of how the foot is built. It’s all about the nerves in the foot.
Foot Structure and Nerve Pathways
The foot has bones, muscles, and nerves. The interdigital nerve is key. It runs between the toes. It can get squished or hurt, leading to Morton’s Neuroma.
The Interdigital Nerve
The interdigital nerve helps us feel our toes. When it gets squished, it hurts. This is what Morton’s Neuroma feels like. For more info, check out Gait Doctor’s page.
Why the Third Web Space Is Often Affected
The third web space gets Morton’s Neuroma a lot. It’s because of the nerve and the stress it gets. Knowing why helps prevent and treat it.
Learning about the foot and Morton’s Neuroma helps us prevent it. It also helps us find the right treatment.
Causes and Risk Factors
Wearing the wrong shoes and how your feet move can cause Morton’s Neuroma. This condition can start from wearing bad shoes, foot problems, and doing certain sports.
Biomechanical Contributors
How your feet move is key in getting Morton’s Neuroma. Problems like overpronation or supination can make your foot uneven. This unevenness puts extra stress on the nerves between your toes.
Footwear Considerations
Wearing high heels or tight shoes can make Morton’s Neuroma worse. Mayo Clinic says that shoes that squeeze your toes can make it worse.
| Footwear Type | Risk Level | Reason |
|---|---|---|
| High Heels | High | Increases pressure on the toes and forefoot |
| Tight Shoes | High | Compresses toes, increasing pressure on nerves |
| Wide, Comfortable Shoes | Low | Reduces pressure on toes and forefoot |
Activities and Sports That May Increase Risk
Some activities and sports can raise your risk of Morton’s Neuroma. Running, dancing, and sports that make your feet move a lot can cause it.
Morton’s Neuroma Symptoms: What to Look For
It’s important to know the signs of Morton’s Neuroma. This helps in getting the right treatment. The condition shows up in the foot with certain feelings and pain.
Common Sensations and Pain Patterns
People with Morton’s Neuroma might feel burning, numbness, or tingling in their toes. These feelings are usually in the ball of the foot. They get worse when you walk or run.
The pain from Morton’s Neuroma can feel sharp, shooting, or burning. It often happens between the toes, like between the third and fourth toes.
Progression of Symptoms Over Time
Left untreated, Morton’s Neuroma symptoms can get worse over time. At first, you might just feel a little discomfort. But as it gets worse, the pain can stay even when you’re not active.
Watching how your symptoms change is key. If they get worse or bother you every day, see a doctor.
When Symptoms Typically Occur
Wearing tight or high-heeled shoes can make Morton’s Neuroma symptoms worse. Running or hiking, which stress your feet a lot, can also make it hurt more.
| Activity | Effect on Symptoms |
|---|---|
| Running | Increased pain due to repetitive stress |
| Wearing tight shoes | Compression of the affected nerve |
| High-impact activities | Aggravation of symptoms due to increased foot stress |
Knowing when and how symptoms happen can help manage Morton’s Neuroma better.
Diagnosing Morton’s Neuroma
To find Morton’s Neuroma, doctors use a mix of checks and sometimes pictures.
Clinical Examination Procedures
First, doctors check your foot. They look at your health history and do a physical check. They might do the Mulder’s click test to see if you have a neuroma.These tests help figure out if you have it and how bad it is.
Imaging Options and Their Effectiveness
Imaging tests can help confirm a neuroma. X-rays show bone problems but not soft tissue neuromas. MRI (Magnetic Resonance Imaging) is better for soft tissue like neuromas. Mayo Clinic says MRI is great for seeing the neuroma’s size and where it is.
Differential Diagnosis: Similar Conditions
It’s key to tell Morton’s Neuroma from other issues that might feel the same. A good check and pictures can help get the right diagnosis. Some similar problems are:
- Stress fractures
- Arthritis
- Nerve entrapment
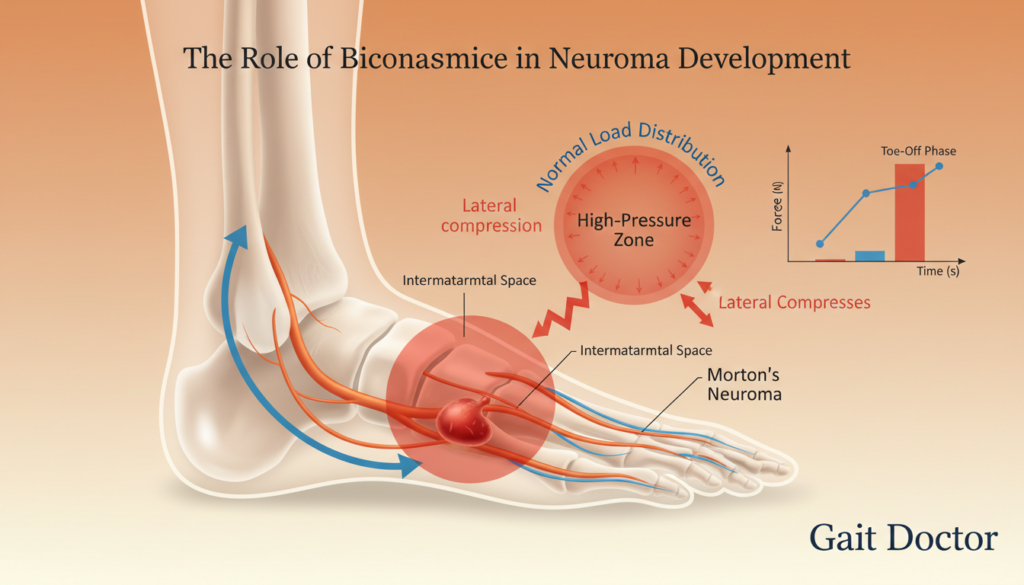
The Role of Biomechanics in Neuroma Development
Foot biomechanics is very important in Morton’s Neuroma. Bad foot mechanics can press on nerves, leading to this condition.
Foot Mechanics and Nerve Compression
The nerve between the toes can get squished if the foot doesn’t move right. Poor foot mechanics put more pressure on the nerve. This causes the pain and numbness of Morton’s Neuroma.
Gait Patterns That May Contribute
How we walk affects Morton’s Neuroma. Bad walking can put uneven pressure on the foot. People with bad walking are more likely to get Morton’s Neuroma.
The Connection Between Foot Structure and Symptoms
The shape of our feet is linked to Morton’s Neuroma symptoms. Foot structure problems, like flat feet or high arches, can cause it.
| Foot Structure | Potential Impact on Morton’s Neuroma |
|---|---|
| Flat Feet | Increased pressure on the interdigital nerve |
| High Arches | Concentration of pressure on the ball of the foot |
| Normal Foot Structure | Less likelihood of nerve compression |
Prevention Strategies for At-Risk Individuals
People at risk can lower their chance of getting Morton’s Neuroma by taking steps ahead of time. It’s very important, mainly for those who often get foot problems or have had them before.
Proactive Footwear Choices
Choosing the right shoes is a big help in preventing Morton’s Neuroma. Shoes with a wide toe box are good because they don’t put too much pressure on your toes. Also, stay away from high heels and tight shoes that can make nerve problems worse.
| Footwear Feature | Benefit |
|---|---|
| Wide toe box | Reduces pressure on toes and interdigital nerves |
| Cushioning | Absorbs shock and reduces stress on foot structures |
| Supportive arch | Helps maintain proper foot alignment |
Activity Modifications
Changing how you do activities can also help prevent Morton’s Neuroma. Try to avoid doing things that put a lot of stress on your feet, like running on hard ground. Instead, choose activities that are easier on your feet, like cycling or swimming.
Early Intervention Approaches
Getting help early is key if you think you might have Morton’s Neuroma. Seeing a doctor right away can stop it from getting worse. They might suggest orthotic interventions or changes to your shoes and activities.
Conservative Management Approaches
Many people choose conservative management for Morton’s Neuroma first. This method helps ease symptoms and improves foot function without surgery.
Footwear Modifications
Changing shoes is a big part of conservative management. Wearing shoes with a wider toe box helps. It reduces pressure on the nerve.
Also, avoid high heels and choose shoes with good arch support. This makes a big difference.
Activity Adjustments for Symptom Relief
Changing daily activities helps manage Morton’s Neuroma symptoms. Doing less high-impact activities like running or jumping helps. It reduces stress on the foot.
Try low-impact exercises like swimming or cycling. They keep you fit without hurting the affected area.
Pain Management Strategies
Managing pain is key for Morton’s Neuroma. Use over-the-counter pain relievers and anti-inflammatory meds. They help a lot.
In some cases, corticosteroid injections are suggested. They cut down inflammation and pain.
Using these strategies can help avoid surgery. It can also improve your life quality.
The Role of Gait Analysis in Assessment
Gait analysis is key in checking Morton’s Neuroma. It finds biomechanical problems that might cause the condition. Doctors look at how a person walks to understand the symptoms better.
How Gait Doctor’s Assessment Process Works
The gait analysis checks how a person walks. Doctors watch how feet, ankles, and legs move. They use tech like video and pressure maps to see gait details.

What a Biomechanical Evaluation May Reveal
A biomechanical check shows many things about walking. It might find issues like uneven weight or bad walking patterns. Doctors use this info to make a treatment plan.
Connecting Movement Patterns to Neuroma Symptoms
Doctors link walking patterns to neuroma symptoms with gait analysis. They find out which movements make symptoms worse. Then, they help change these movements to feel better.
Orthotic Interventions and Support Options
Orthotics help a lot with Morton’s Neuroma. They give support and ease the pressure on the nerve. If you have symptoms, orthotics can be a big help in your treatment plan.
Over-the-Counter Support Solutions
OTC orthotics are easy to find and can help right away. They make your foot feel better by spreading out the pressure. You can find arch supports and metatarsal pads that work well.
Custom Orthotic Considerations Following Assessment
If you need something special, custom orthotics might be right for you. They are made just for your foot. They help your foot feel better and can slow down Morton’s Neuroma.
How Orthotics May Help Address Underlying Factors
Orthotics can fix many problems that cause Morton’s Neuroma. They help your foot feel stable and spread out the pressure. This makes your foot feel better.
Potential Benefits for Some Individuals
Orthotics can really help some people. They can make it easier to do everyday things without pain. Always talk to a doctor to find the best orthotics for you.
Limitations and Realistic Expectations
Orthotics are great, but they’re not perfect. They might not work for everyone. You might need to change your shoes and how you move to get the best results.
| Orthotic Type | Benefits | Considerations |
|---|---|---|
| Over-the-Counter | Immediate relief, affordable | May not address specific foot needs |
| Custom Orthotics | Tailored support, addresses unique foot structure | Requires professional assessment, potentially more costly |
Knowing about different orthotics can help you choose the right one. Always talk to a doctor to find the best orthotics for you.
Conclusion: Managing Morton’s Neuroma Long-Term
Managing Morton’s Neuroma needs a mix of treatments. This includes both non-surgical and surgical options. Understanding the condition and its causes is key to managing it well.
A good plan includes choosing the right shoes and changing how you move. Orthotics can also help. These steps can lessen the pain and discomfort.
Preventing Morton’s Neuroma is important. Wearing the right shoes and staying healthy can help. These steps can lower your risk of getting it or having it get worse.
With the right management, you can live a full life. You can do things you love without pain. Use what you learned here and talk to a doctor to make a plan that’s just for you.